Defeating Diabetes with Technology
UCSB-Sansum Team Creating Artificial Pancreas
People who suffer from type 1 diabetes are closer than ever to ending their constant blood sugar-monitoring and insulin-dosing regime, and, as of this month, those diabetics on the very frontier of this breakthrough are now walking among us, playing bocce while waiting for dinner at Arnoldi’s, dabbling at keyboards in the Apple Store on State Street. These select few are participating in the first round of outpatient clinical trials for an artificial pancreas, which was developed by a team of UCSB engineers and doctors at Santa Barbara’s Sansum Diabetes Research Institute, whose founder, Dr. William David Sansum, was the first in America to inject insulin as a treatment for diabetes in the 1920s.
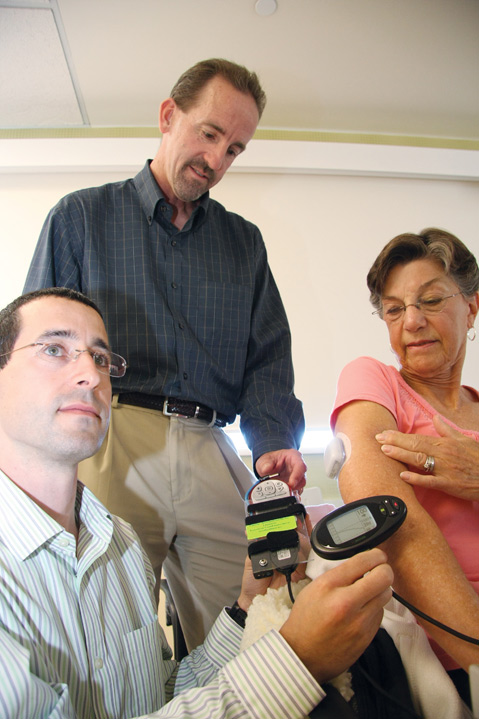
“This is a treatment and not a cure, but a treatment that lends itself to an improved lifestyle and an extended life using basic engineering technology,” said Professor Frank Doyle of UCSB’s Chemical Engineering department, who leads the artificial pancreas team and is hopeful this will become available to the public soon. “I’ve always said five to 10 years, but I say now that we are inside the five-year envelope for sure.”
Type 1 diabetics — many of whom develop the disease as children — cannot produce insulin, which is what breaks down glucose to fuel the body. Type 2 diabetics, whose disease is often lifestyle-caused, can produce but cannot process insulin. So scientists have developed a glucose monitor to check blood sugar every few minutes as well as the insulin pump, which started replacing the syringe injections over the past decade. But because the body’s chemistry is so unpredictable, varying widely due to stress, anxiety, illness, and other causes, it’s been challenging to develop a reliable, accurate way for the glucose monitor to tell the pump when to release insulin, a drug with both acute and chronic impacts when misused. “Insulin, while life-enabling and hugely therapeutic, is potentially a toxic drug,” said Doyle. “You’re walking this tightrope between giving just enough to help somebody and potentially putting them in a coma or worse.”
Doyle’s group is focused on a completely automatic solution that removes a patient’s intervention in the process — which is strategic, considering many are young kids who may not follow protocol — and uses an algorithm tailored specifically for each patient, which can be altered per doctor’s orders. For meaningful success, Doyle believes, “You have to make the technology invisible, like an artificial heart.” With outpatients walking the streets of Santa Barbara thanks to federal approval for the trials this month, the end zone seems finally in sight.
“Currently, the management of type 1 diabetes is absolutely relentless,” said Katheryn Keller, whose father died from the disease which prompted her involvement with the Juvenile Diabetes Research Foundation (JDRF), which has given $3.5 million in recent years to support Doyle’s work. “From infants to the elderly, patients must constantly balance insulin delivery against a multitude of factors … . This technology will bridge that gap.”
Explaining that his research group is “one of the most powerful” of the roughly 10 teams across the world focused on this gap, Doyle said he started working on the idea 20 years ago but that the work “really accelerated” when, in 2002, he came from Purdue to UCSB, where a cross-disciplinary culture thrives. “The signature of our team is that we have doctors and engineers shoulder-to-shoulder,” said Doyle. “In a lot of places, doctors throw the data over the fence to engineers, and the engineers throw software and code over the fence to the doctors. We have doctors who are adjunct faculty on campus, and we have faculty who are investigators at the clinic.”
Actually curing type 1 diabetes still remains the biggest hope for this community, but until then, the artificial pancreas is looking pretty sweet. “Curing diseases is not an easy thing,” said Doyle. “But we realize that, with technology, we could make the lives of people with this disease much better.”
4•1•1
The Juvenile Diabetes Research Foundation’s three-mile Walk to Cure Diabetes, which helps fund the artificial pancreas project, is on Saturday, October 12, 10 a.m. See walk.jdrf.org/santabarbara to register.



