In Vitro Fertilization, Part II: Consequences
One in a Hundred American Babies
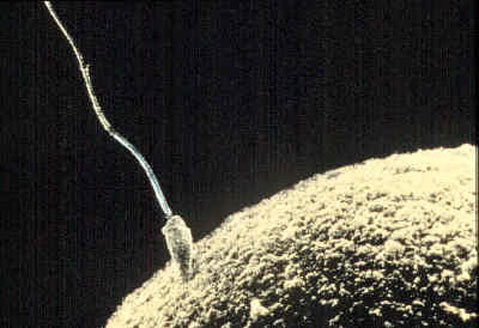
The technology has come a long way since in vitro fertilization (IVF) was first successfully used in humans, resulting in the birth of Louise Joy Brown in 1978.
Today, over one percent of the births in the United States are due to IVF. However, the practice has also gained a lot of baggage along the way. Here, we will explore the many social, legal, and economic consequences of widespread use of IVF.
Last week in “Biology Bytes,” we explored the history and biology of in vitro fertilization, which will be summarized here. IVF is often used by people who desire to have their own biological children, but are unable to do so due to fertility problems. In IVF, sperm and eggs are removed from donors and fertilized outside of the body, in a controlled laboratory environment, and then the fertilized eggs are implanted into a recipient woman. This is, of course, an oversimplification: A variety of options can be available to someone interested in IVF, from what to do with extra embryos, to selecting for certain genetic traits, to choosing to have the pregnancy “outsourced,” and much more.
Frozen Embryos Embryos have been frozen and successfully used in pregnancies since the early 1980s While there is a slightly lower pregnancy rate, there are no clear differences in the occurrence of abnormalities in children born from frozen versus fresh embryos. Why would a couple choose to freeze their embryos? If the first IVF cycle doesn’t work, freezing makes it quicker to try a second cycle; or the embryos could be used much later to potentially create another child. However, because so many couples freeze their embryos, there are now over half a million frozen embryos in the U.S. Many wonder what to do with these embryos, which could be donated to another couple or used for valuable research, such as the creation of embryonic stem cells.
Embryonic stem cells In 1998, researchers led by Dr. James Thomson (who holds a faculty appointment at the University of Wisconsin and locally at UC Santa Barbara) first isolated human embryonic stem cells (hESCs) from early-stage embryos (four or five days post-fertilization). Because hESCs can become virtually any cell type, they have great potential for studying and curing diseases and injuries, and, theoretically, creating organs.
These early-stage embryos were from IVF clinics and donated with full consent. The embryo contains approximately 150 cells at this point and is a hollow, fluid-filled sphere.
Often the embryos used to create hESCs would have otherwise been discarded by IVF clinics because they were abnormal, though it’s since been shown that hESCs can be made from a small piece of a normal embryo, and that embryo can still normally mature.
Designer Babies One of the most controversial recent developments of IVF is using it to select for certain genetic traits in embryos, and, consequently, children. How is this done? After sperm and eggs are removed from the donors, the sperm is allowed to fertilize the eggs and the resultant embryos (when they reach three days old) can have one cell safely removed to perform genetic testing on their DNA.
One form of genetic testing is called “preimplantation genetic screening” (PGS), which counts the number of chromosomes in the embryo’s cell. If a woman is over 35 years old, her eggs have a significant chance of having genetic abnormalities. Specifically, a person normally has 23 pairs of chromosomes (for a total of 46 chromosomes), but embryos made from an egg with genetic abnormalities may have an extra copy of one chromosome, resulting in a “trisomy” (three copies of one chromosome instead of two copies). Or, instead of a pair of chromosomes they may have only one. Most of these anomalies are lethal, which can cause repeated miscarriages. An exception is Down Syndrome, which is caused by three copies of the chromosome labeled “21,” and is why it is also called Trisomy 21. PGS allows couples to prevent implanting an embryo with any of these genetic maladies.
Taking this a step further, IVF can allow prospective parents to select for, or against, specific genetic traits through preimplantation genetic diagnosis (PGD). One of the least controversial uses of PGD is screening against an embryo inheriting a high-risk genetic disorder from the parents. One of the many couples who have used PGD in this manner are Susan and Chris Paget Dunthorne in the UK. Mr. and Mrs. Dunthorne’s first child died when he was only a few months old, having inherited cystic fibrosis from the couple; they had not known they were carriers. The couple wanted to make sure their next child did not have the devastating disease, and did so by undergoing IVF and having their embryos screened for this genetic condition. Eventually, Susan had a healthy son through IVF and PGD.
PGD has also been used to select the gender of an embryo, though mainly for preventing a sex-linked genetic disease from being transmitted. Social, rather than medical, reasons are usually what stops this practice. One clinic, The Fertility Institutes in the U.S., started advertising to do genetic screening for couples to select specific hair and eye color, as well as complexion and gender, but halted the campaign (except for gender selection) after much public backlash.
More controversially, PGD has been approved to create “savior siblings.” Raj and Shahana Hashmi, from the UK, had a son, Zain, who suffered from beta thalassaemia, a blood disease with severe symptoms; he would require painful, life-long medical care or have a life expectancy of a few years. Because umbilical cord blood from a baby of the same tissue type could save Zain, Zain’s parents decided to have another child using IVF, and find a match by screening for a human leukocyte antigen which determines tissue type. While their choice was approved by governing bodies, the IVF attempts were not successful. The Hashmis continue to look for matching bone marrow donors for Zain.
Legalities of IVF In the U.S., there is a striking lack of uniformity in laws and regulations surrounding IVF. The laws vary from state to state and there are very few federal laws. For donating eggs or sperm, the American Society for Reproductive Medicine has created guidelines to ensure safety tests are performed on the donated material, but that’s it. Additional requirements for donors differ between states.
There are great differences even between banks in the donor information provided to prospective recipients, as well as the requirements for recipients. For example, some require that recipients be married or heterosexual, while others do not.
Paternity questions are often raised. While people can create documents that waive the donors’ parental rights, only a few states assure that the contracts are legally valid. Such parental claims are often resolved in private agreements or courts.
Laws have been gray over who can claim ownership of sperm or eggs to be used in IVF. As a result of multiple instances where sperm was collected from dead or comatose men whose spouses (or significant others) then wished to undergo IVF using the genetic material, the UK has made it illegal to remove, store, or use anyone’s gametes in the UK without the donor’s written consent.
Individuals seeking to use even their own gametes have come up against legal difficulties. For example, in 1999, 24-year-old Carolyn Neill in the UK had cancer and found she would have to undergo chemotherapy. Because this would most likely leave her infertile, and she had not had children, Neill decided to have some of her eggs frozen. After the chemotherapy treatment was successful, Neill found that she could not retrieve her eggs because using thawed eggs in IVF had not been successful in the UK yet, and consequently such practice was illegal.
However, fearing human rights litigation, the ban on using frozen eggs was eventually lifted. While the success rate is still quite low, children born from frozen eggs have not been shown to have any more abnormalities than children born naturally.
Multiple Births One of the highest risks associated with IVF is having multiple children from one pregnancy. About 24 percent of all IVF births are twins or triplets. However, this can be regulated by controlling how many embryos are implanted in the recipient’s uterus.
In the UK, usually one or two embryos are implanted, and a healthy woman of childbearing age has about a 28 percent chance of pregnancy from one IVF cycle. Because the successful pregnancy rate for older women is lower, women over 40 can have three embryos implanted at once, the legal maximum in the UK. (It should be noted that although a menopausal woman cannot naturally become pregnant, her uterus can still be prepared to successfully receive an embryo through IVF, leading to many publicized mothers in their 60s and 70s.)
In the U.S., the American Society for Reproductive Medicine gives similar guidelines, recommending that women under 35 have one or two embryos implanted at once, and that women 35 to 40 be implanted with three at most, bumped up to a maximum of five for women over 40.
However, even though the ASRM has “guidelines,” the U.S. does not have any federal restrictions on the number of embryos that can be implanted in a woman during one IVF treatment. This led to 33-year-old Nadya Suleman, the famous “Octomom,” having octuplets in 2009 (in addition to the six older children she also conceived through IVF).
Multiple births are also associated with a higher risk of miscarriages. In 1996, Mandy Allwood, who had been taking fertility drugs, became pregnant with octuplets (though not through IVF). Despite the strong recommendations of doctors to undergo selective abortions to help some of the fetuses survive, Allwood continued with the pregnancy and all of the octuplets were lost in a miscarriage when Allwood was 19 weeks pregnant. Federal regulation of the number of embryos that can be implanted during IVF may help decrease the number of multiple births associated with it, which can result not only in miscarriages but in women having far more children than they’d planned for.
Surrogacy and “Outsourcing” Pregnancy Similar to the legal problems surrounding IVF in general, laws surrounding surrogacy in the U.S. differ by state—especially the rights of surrogates, donors, and “intending parents.” In some states surrogacy is banned. But where it is allowed, usually a contract is created between the involved parties, and when conflicts have arisen, the “intending parents” have usually ended up with the baby.
However, this is not always the case. One such instance involved a British woman who carried a baby for a Californian couple, using embryos fertilized through IVF. When the woman became pregnant with twins, and refused to have one fetus aborted, as the couple requested, the couple reneged on the contract and the British woman ended up with two new children.
Like many jobs, surrogacy is also increasingly becoming “outsourced.” A booming surrogacy industry has taken root in India, where surrogates incubate babies for couples in European countries, the United States, or other countries. In India, a surrogacy that could cost up to $70,000 in the United States can cost only $12,000. At the forefront of this industry is the Akanksha Infertility Clinic in Anand, where pre-screened women are paid $5,000 to $7,000 for each pregnancy. Interested recipients can either have their own sperm and eggs implanted, or use donor gametes. For the well-being of all parties involved, many feel this outsourced practice needs to be much more tightly regulated, especially since different countries have very different laws on surrogacy.
Potential Consequences for Coming Generations While IVF allows people to have children, when they may not have been able to otherwise, adding a net gain to the global population, there are concerns that increased use of IVF may actually be propagating infertility genes. Infertility is often caused by genetic abnormalities, frequently in the male factor, which are easily solved by intracytoplasmic sperm injection, as discussed previously. However, it’s generally recommended that discriminating against potential IVF clients on the basis of genetics be avoided, because of its eugenic undertones.
Many of the questions and concerns surrounding the multifaceted nature of IVF may be resolved in courtrooms as its use becomes more widespread. Perhaps eventual federal solutions will put interested parties more at ease regarding what to expect, helping smooth some of the bumps on the emotional rollercoaster.
For more on in vitro fertilization, see the book From IVF to Immortality by Ruth Deech and Anna Smajdor, the book Test Tube Families: Why the Fertility Market Needs Legal Regulation by Naomi R. Cahn, the book In Vitro Fertilisation in the 1990s by Elisabeth Hildt and Dietmar Mieth, the Center for Disease Control’s website on the 2007 Assisted Reproductive Technology Report, Medical Tourism Corporation’s detailed website on Low Cost Surrogacy in India, the websites of the Akanksha Infertility Clinic, Surrogacy Abroad in India, the ABC World News report ”More Americans Now Traveling to India for Surrogate Pregnancy”, or Wikipedia’s article In vitro fertilization”.
Biology Bytes author Teisha Rowland is a science writer, blogger at All Things Stem Cell, and graduate student in molecular, cellular, and developmental biology at UCSB, where she studies stem cells. Send any ideas for future columns to her at science@independent.com.



